Background
According to the Department of Defense, between 170,000 and 240,000 people join the military each year in the Active and Reserve components. According to the Department of Veterans Affairs (VA) in 2018, approximately 200,000 veterans transitioned to their new roles as civilians.
When individuals leave home to attend basic training, they are asked to strip elements of their individuality. In exchange, they are issued pay, uniforms, and a new community. Within this new community, service members learn the importance of rank, leadership traits, and the benefits of working as a team. This new community provides a sense of belonging and purpose, which grows as service members progress in their military careers.
When service members arrive at their first duty station, they become part of a new community where they will work, live, exercise, and in some cases, leave their loved ones and deploy together. They will also have their medical needs met and are given clear instructions on how to access assistance. As service members accumulate years of service and attain higher rank, their stature within their communities becomes more significant. Through each stage of their career, service members have connections with mentors who help them cope with career progression, medical needs, leadership challenges, family life, and many other issues professional and personal issues.
Issue
Upon leaving active duty, many veterans look to the VA to provide the physical and behavioral health resources that were previously provided while in the military. Unfortunately, community health resources are not part of the VA’s list of services. Community health refers to the veteran’s ability to find a new community, develop healthy relationships, and adjust to the culture. The new challenge for veterans becomes finding that same sense of belonging and purpose that was part of the military community.
Finding the right combination of physical, behavioral, and community health resources can be difficult for some while it comes naturally for others. For those that struggle with the transition out of the military, finding a new community feels impossible as veterans leave a structured lifestyle and make sense of their path in civilian society. These issues are brought to light in a 2015 study from the Institute for Veterans and Military Families (IVMF), who listed the five major challenges in the transition from military to civilian life:
- Navigating VA programs, benefits, and services (60%)
- Finding a job (55%)
- Adjusting to civilian culture (41%)
- Addressing financial challenges (40%)
- Applying military-learned skills to civilian life (39%)
The challenge of transitioning to civilian life does not include a scarcity of resources. In fact, the issue is quite the opposite, with thousands of organizations advertising their services for helping veterans. For instance, the VA’s My Health E Vet platform has 21 applications that are dedicated to helping veterans find mental health resources. The VA has also developed the National Resource Directory (NRD), a database of vetted resources for veterans based on location and need.
Additionally, the Guidestar nonprofit database provides information for every registered nonprofit across the country. When searching this database using the term “military”, there are over 93,000 results. When searching the database using the term “veteran”, there are over 69,000 results, meaning there are over 69,000 veterans-serving organizations (VSOs) across the country, not including government agencies.
Given the vast number of resources, veterans must dedicate themselves to navigating through the large volume of available information to develop a plan that fits the needs of themselves and their families. Navigating the maze of nonprofits, federal agencies, state agencies, and corporate resources can be infuriating and overwhelming, but not impossible with the right methodology, guidance, and planning efforts that occur well in advance of transition to civilian life.
Solution
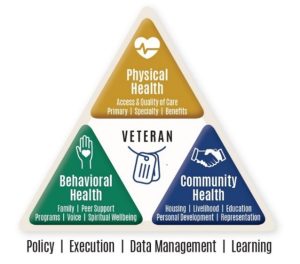
Both veterans and the VA must strongly consider the importance of interconnectedness with physical, behavioral, and community health resources and their effects on the veteran’s wellness. The graphic shown in Figure 1 was developed by RB Management Consultants (RBMC) and teammate, A-G Associates, to represent the Veteran Wellness Model. This model is grounded in both research and first-hand experience.
The objective of this model is to highlight the necessary components of veterans holistic wellness and illustrate the connection between each component. The model can be used by veterans and the VA when looking to navigate, and categorize, the vast number of VSOs, and the value they bring to the veteran community.
Veterans
Veterans should use this model to evaluate whether their health and wellness needs are being met. The model can be used as a guide to help veterans and their families facilitate important conversations and answer critical questions that will help uncover which areas are strong within their support system, and where additional resources may be needed. For the questions that do not have favorable responses, veterans can identify specific areas that need attention, which narrows search criteria and makes the task of finding resources less overwhelming. Critical questions may include:
- Physical Health: Do I have adequate healthcare resources to fit the needs of myself and my entire family? What are the limitations to my benefits with the VA versus private providers? This is important for those whose VA benefits are limited or live in areas where VA clinics are inaccessible. For those with special needs, the access to care and specialty resources will be a critical consideration.
- Behavioral Health: Do I have an adequate support system with my family, peers and/or professionals? Can I effectively deal with stressful situations? This aspect is a key component for helping the veteran cope with the stress that comes along with losing his/her role in the military.
- Community Health: Do I have a sense of purpose and feeling of belonging? Am I in a job where I see a clear career path? Is my voice represented in my community? This aspect is often overlooked, but can be a major stressor in the veteran’s life. This includes finding employment that serves financial needs, but also offers a culture of personal development, camaraderie, and teamwork. This also includes finding social supports that address the need for being part of a group.
VA
The VA can also use the model to identify areas where they play an important (lead) role and where they need the cooperation of the veteran service provider community. The VA can then engage the necessary stakeholders to develop an integrated plan with a shared vision and goals.
This model will allow the VA to develop well-informed policies, execute those policies collaboratively with the cooperation of the VSO and stakeholder communities, manage the critical components of data that will provide meaningful evaluation and feedback, and provide learning opportunities for all parties. This solution becomes extremely important when looking at the implementation of the Mission Act and when the VA must engage the private healthcare provider community to ensure veterans and caregivers have adequate health resources.
For more information about the Veteran Wellness Model or Team RBMC, please contact Chris Gonzalez (information below) or visit http://rbmanagementconsultants.com. Team RBMC provides data-driven solutions and has worked with several public and private healthcare systems, and managed care organizations, to engage their stakeholders, analyze population-health needs, and address social determinants of health.
About the Authors
Chris Gonzalez is the President of A-G Associates, a Service-Disabled Veteran-Owned Small Business. Chris is a combat veteran with tours in Iraq and Afghanistan as a U.S. Marine. Chris currently serves in the Reserves as an instructor at the Marine Corps Security Cooperation Group and previously served at the Marine Corps Civil Military Operations School. You may reach him by email at cgonzalez@a-gassociates.com.
RB Management Consultants is a CVE certified Service-Disabled Veteran-Owned Small Business with more than 60 years of experience supporting public, private, and non-profit clients in over 50 countries, with a focus on healthcare transformation. You may reach them by email at contact@rbmanagementconsultants.com.
HCAM Services
- If you are in need of health insurance, HCAM’s certified navigators can assist you this Open Enrollment (Nov. 1 – Jan. 15th) in finding the right plan for you. Call 410-500-4710 to schedule your appointment today.
- HCAM’s Here2Help Hotline provides free, confidential advice and emotional support and is available 24/7, 365 days a year. Trained mental health specialists are available to listen and connect you or a loved one to mental health and substance use disorder services. Call 410-433-5175 to be connected to a trained mental health specialist. The Here2Help Hotline is a partnership between HealthCare Access Maryland, Baltimore Crisis Response, Inc. and Behavioral Health System Baltimore.






